- About us
Mō mātou
About us
- Our work
Ngā mātou mahi
Our work
- About bleeding disorders
Mō ngā raru ā-toto
About bleeding disorders
- How you can help
- News & research
Ngā pitopito kōrero, ngā rangahau hoki
News & research
- Members area
Te taunga ā-mema
Members Area
von Willebrands Disorder
Von Willebrands Disorder is a blood clotting condition, which is usually inherited. It is sometimes known as von Willebrands disease or just vWD. Research has shown that as many as 9 out of 10 people with vWD have not been diagnosed.
One of the factors in our blood that helps form blood clots is von Willebrand factor. It acts as glue, sticking platelets to the wall of a broken blood vessel. People with vWD have limited von Willebrand factor. vWD is the most common bleeding disorder in the world, and is thought to affect approximately 1 in every 100 people.
Although similar to haemophilia, people with vWD usually suffer more from prolonged external/skin bleeding, rather than internal bleeds. The disorder is passed on through an abnormal gene that can be inherited from the mother or father (or both, in some cases).
Types of vWD
vWD can affect both sexes and there are a number of different sub-types.
There are three main types of vWD. Within each type, the disorder can be mild, moderate, or severe. Bleeding symptoms can be quite variable within each type depending in part on the VWF activity. It is important to know which type of vWD a person has, because treatment is different for each type.
Type 1 vWD
Type 1 vWD is the most common form. People with Type 1 vWD have lower than normal levels of normally functioning VWF. Symptoms are usually very mild and many people with vWD will lead normal active lives, with no need for treatment. Symptoms can include regular nosebleeds, bruising, and in women, heavy periods. Still, it is possible for someone with Type 1 vWD to have serious bleeding, especially after trauma or surgery.
Type 2 vWD
Type 2 vWD involves a defect in the structure of the person's von Willebrand Factor (vWF). The vWF protein does not work properly, causing lower than normal VWF activity. There are different Type 2 VWD defects. Symptoms are usually moderate and can include regular nosebleeds, bruising and, in women, heavy periods. Some sub-types, such as 2b or 2n, are quite.
Type 3 vWD
Type 3 vWD is usually the most serious form of the disease. People with Type 3 vWD have very little or no vWF. Symptoms are more severe. In addition to symptoms associated with milder forms of vWD, people with Type 3 vWD can have bleeding into muscles and joints, sometimes without obvious injury as they also have low levels of factor VIII, like people with haemophilia A.
vWD Inheritance
You are born with vWD. It is usually passed down through the genes, it can come from either parent, and can affect a child of either sex.
As vWD is hereditary. There is usually evidence of a family history of bleeding problems, but the symptoms of vWD can vary a lot within a family, and sometimes be so mild so that it is not recognised. Sometimes vWD occurs due to a spontaneous change in the vWD gene before the baby is born.
vWD Types 1 and 2 are usually inherited in what is known as a "dominant" pattern. This means that a parent who has vWD has a one in two (50%) chance of passing a VWD gene on to each of his or her children.
Type 3 vWD, however, is usually inherited in a "recessive" pattern. This type occurs when the child inherits the gene from both parents. Even if both parents have mild symptoms or no symptoms at all, their children may be severely affected.
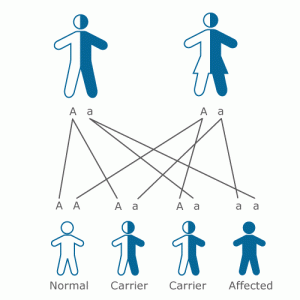
Recessive Inheritance
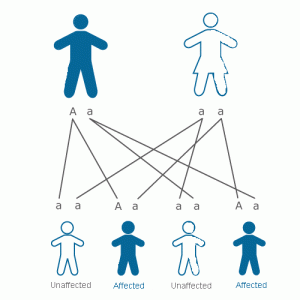
Dominant Inheritance
vWD Diagnosis & Treatment
The first indications of vWD may be noticed after a minor surgical procedure (such as a tooth extraction), where prolonged bleeding might be observed. Other symptoms may include frequent nosebleeds, heavy menstruation, and bleeding after invasive surgery.
If vWD is suspected, your doctor can arrange tests to determine how long you bleed before your blood clots and blood tests to measure your level of von Willebrand factor. Your doctor will also take into consideration your personal and family medical history.
The type of treatment depends on the individual, their type of vWD and the severity of the bleeding. Treatments may have side effects and the right course of action should be decided on in consultation with a doctor.
People with mild forms of vWD often do not require treatment for the disorder, except at times of higher risk such as surgery or dental work. Minor bleeds can often be treated with the P.R.I.C.E. regimen (Protect. Rest. Ice. Compression. Elevation).
For those with more serious bleeds or who need further treatment there are several options, depending on individual circumstances and the severity of the disorder. Desmopressin (often just called DDAVP) is a synthetic drug, which copies a natural hormone that acts by releasing von Willebrand factor stored in the lining of the blood vessels. People react to desmopressin is different ways and a doctor will need to test an individual’s response to the drug before there is an urgent need for the drug, such as surgery. A sufficient amount of time, usually 48-72 hours, must pass between doses to allow the body to rebuild its stores of von Willebrand factor. Desmopressin can also have mild side effects such as facial flushing, headache, nausea, and water retention. You will need to have a restriction on oral fluids for 24 hours after using DDAVP. How much fluid you are able to have varies based on age and size. Your HTC will be able to advise. Desmopressin is generally avoided in those with known cardiac issues, and those over 65. It can be used in pregnancy and in the very young, but this needs assessment in conjunction with your HTC, as it is not as straight forward as in other groups.
People with Type 3 vWD and some forms of Type 2 vWD often need factor replacement with factor concentrates. Plasma-derived Factor VIII concentrate also contains vWF. Recombinant vWF has been developed but is not yet available in New Zealand. Factor concentrates are also used when desmopressin is not effective or when there is a high risk of major bleeding, such as for major surgery.
Bleeding in mucous membranes (inside the nose, mouth, intestines or womb) can be controlled by drugs such as tranexamic acid, aminocaproic acid, or by fibrin glue. However, these products are used to maintain a clot and do not actually help form a clot.
Hormone treatment, such as oral contraceptives (birth control pills), can help increase VWF and Factor VIII levels and control menstrual bleeding. If hormone treatment is not prescribed, antifibrinolytic agents may be effective for treating heavy menstruation. HTCs will often refer woman with significant menstrual bleeding to a gynaecologist for specialist input on possible treatments. Women who suffer from anaemia (low levels of iron in the blood, causing weakness and fatigue) due to excessive menstrual bleeding may need to take iron supplements.